Opioids
1. General Information About Opioids

Opioids are medications that are prescribed primarily to relieve pain. When used properly, they can help. But misuse can cause dependence, overdose and death.
Opioids that are prescribed as medications include codeine, morphine, oxycodone, and hydromorphone. If you have been prescribed an opioid medicine, it should:
- Only be taken as prescribed;
- Never be used by someone for whom it was not prescribed; and
- Never be taken with alcohol or other medications (except as prescribed).
Keep your medication safe to help prevent problematic use by others by:
- Never sharing your medication with anyone else. This is illegal and may also cause serious harm or death to the other person;
- Keeping track of the amount of pills remaining in a package; and
- Storing opioids in a safe and secure place, out of the reach of children and teenagers.
Unused portions of opioid medicine should always be:
- Kept out of sight and reach of children and pets;
- Stored in a safe place to prevent theft, misuse or accidental exposure. This prevents any possibility of illegal use and protects the environment from contamination; and
- Returned to a pharmacy for safe disposal if it is no longer needed or is expired.
Fentanyl

Fentanyl is an opioid that is 50-100 times more toxic than other opioids (such as heroin, oxycodone and morphine). Doctors may prescribe fentanyl for severe pain and for some medical procedures. Because of the strength of this drug, a health care provider must very carefully monitor the dose to make sure that the person does not overdose.
Legal, prescribed fentanyl is dangerous when not used properly.
Illicit or street fentanyl is not received by prescription. It's sometimes sold by dealers as another drug or mixed into other substances like oxycodone or cocaine. This is when using the drug becomes extremely dangerous; it can slow down a person's breathing, lead to a coma and even death.
For more information:
- Fentanyl - Advisory for Saskatchewan Health Care Providers
- Opioids (Government of Canada website)
- Prescription Medications
- Opioids Video
2. Preventing Opioid Overdoses - Take Home Naloxone
Preventing Opioid Overdoses
In addition to having a naloxone kit readily available, there are other ways to prevent opioid overdose deaths.
If you have been prescribed an opioid medication, it should:
- only be taken as prescribed; and
- never be taken with alcohol or other medications (except as prescribed).
The best way to stay safe is to not use illegal drugs at all. People who do use illegal drugs should:
- test your drugs for fentanyl and benzos using a Take Home Drug Checking Strip; and,
- know that mixing drugs and/or alcohol could lead to an overdose.
If you are alone while using drugs, call the National Overdose Response Service hotline at 1-888-688-NORS(6677) for a volunteer who will stay on the line with you and call for help if you need it.
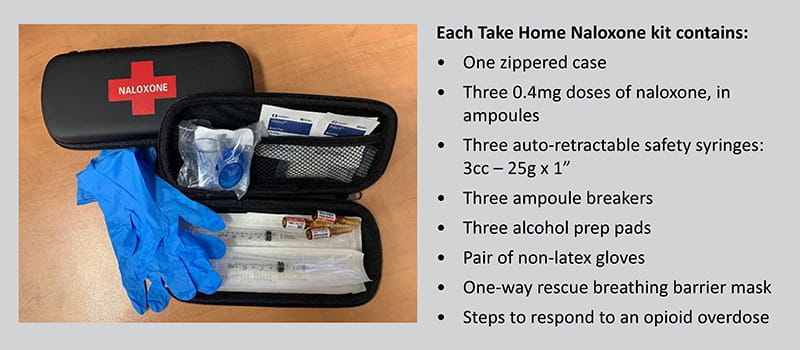
Take Home Naloxone
Naloxone reverses the effects of an opioid overdose temporarily, restoring breathing in a few minutes and buying time for Emergency Medical Services (EMS) to arrive. Saskatchewan residents who are at risk of an opioid overdose and/or might witness an opioid overdose, such as friends and family of people who use opioids, are eligible for free training and a free Take Home Naloxone kit. The training covers overdose prevention, recognition, and response, including how to administer naloxone.
Naloxone does not reverse the effects of non-opioids, such as xylazine, which may be found in street drugs, but Naloxone will still reverse the effects of the opioid, so it is recommended to administer Naloxone in the event of an overdose.
It's important to note that Naloxone treatment itself does not replace the need to seek immediate medical attention. Call 911 immediately if you suspect an overdose.
To find a Take Home Naloxone Program near you call HealthLine 811 or view the Take Home Naloxone Program map.
Naloxone is also available for purchase at pharmacies across Saskatchewan. The Pharmacy Association of Saskatchewan has a list of pharmacies that carry naloxone.
Naloxone is also available for free for First Nations and Inuit clients covered by the Non-Insured Health Benefits Program.
3. Check Your Drugs
Drug checking is testing your drugs for substances you don’t expect and that could be harmful, not testing your urine or blood for drugs. Drugs are checked using fentanyl and/or benzodiazepine test strips. To perform a test, the drug checker will take a tiny sample of the street drug being tested and dissolve it in water. The test strip is then dipped into the water and within a few minutes it will give the result. Coloured lines will appear on the strip indicating a positive result (one line) or negative result (two lines).
The test has some important limitations:
- Fentanyl strips only test for fentanyl, and benzodiazepine strips only test for benzodiazepines within the sample provided.
- Although the sample may be negative, the tested drug may still be present in the remainder of the drug batch.
- Strips may occasionally report a negative result when the drug tested for, or an analogue, is present.
It is important that other precautions are taken, even if your drug checking result is negative.
To find substance checking services, visit the SHA.
Other printable resources:
- Drug Testing - Pamphlet
- Fentanyl Testing Strips - Labels:
- Benzodiazepine Testing Strips - Labels:
- How to use Fentanyl Drug Checking Strips
- How to use Benzodiazepine Drug Checking Test Strips
4. Good Samaritan Act
The federal Good Samaritan Drug Overdose Act provides legal protection for individuals who seek emergency help during an overdose, or who witness an overdose.
5. Treatment, Services and Recovery
When someone has an opioid use disorder, they feel that they need the drug and it can become very hard to quit. When they stop using the drug, it can cause them to feel pain, anxiety or crave more opioids. They might feel shaky, weak, and nauseous; have fever, chills, muscle aches or bone pain; and experience changes to bowel function, sleeplessness, sweating, irritability and vomiting.
There are a variety of treatment options for people with opioid dependence. Opioid Agonist Therapy (OAT) provides treatment for individuals with use disorder dependence. The Saskatchewan Health Authority provides OAT services, which include OAT clinics, Rapid Access to Addiction Services, and Virtual Access to Addiction Medicine across the province.
For more information, and to get help:
- Call HealthLine 811
- Find mental health and addiction services closest to you
- Learn about services available in Saskatchewan to help you deal with alcohol and drug issues
6. Practice Infection Prevention
Getting tested is part of a comprehensive public health infection prevention strategy to reduce the spread of HIV, HCV, and other sexually transmitted and blood-borne infections.
Get more information on testing and treatment.
7. What We're Doing
In November 2018, the Government of Saskatchewan signed a bilateral agreement under the Government of Canada's Emergency Treatment Fund.
In October 2023, the Government of Saskatchewan released a new Action Plan for Mental Health and Addictions that will create 500 new addictions treatment spaces and a central intake system to make care more accessible and responsive.
The new Action Plan has three pillars of focus: building capacity for treatment, improving the system itself, and transitioning to a recovery-oriented system of care for addictions treatment.
As part of this work, a new 60-bed inpatient addictions treatment facility named EHN Willowview opened at the former Living Skies Retreat & Conference Centre near Lumsden. The facility, located about 20 minutes northwest of Regina, provides adults 18 and older with holistic, wrap-around inpatient addictions treatment for up to 16 weeks. EHN Willowview brings the total number of addictions treatment spaces that have been announced under Saskatchewan's Action Plan for Mental Health and Addictions to 264. This includes 26 post-treatment spaces at St. Joseph's Addiction Recovery Centre in Estevan, 32 intensive outpatient treatment spaces through Possibilities Recovery Centre in Saskatoon, 14 inpatient addictions treatment spaces at the Battlefords Treatment Centre in North Battleford, 15 withdrawal management spaces at Onion Lake, 40 mobile withdrawal spaces with Medavie Ambulance in Saskatoon, 20 spaces at Thorpe Recovery near Lloydminster, 15 spaces at Muskwa Lake Wellness Camp, and 42 virtual spaces through EHN Canada.
Work is also underway to implement a central intake system that patients can contact directly to refer themselves for addictions treatment services. A central intake will make the system more accessible to patients and enable care providers to better coordinate care for patients across the system and throughout patients’ care and recovery journey.
Statistics on opioid related harms in Saskatchewan
The Government of Saskatchewan continues to monitor drug related harms to inform our response activities.
Data on the number of drug toxicity deaths in Saskatchewan is available from the Saskatchewan Coroners Service.
National reports on opioid drug use and its impacts, which include data from Saskatchewan, are available from the Government of Canada.
The Canadian Institute for Health Information (CIHI) also has information related to overdose.
